State commits to renewing signature health coverage program; asks for historic waiver.

(Indianapolis, Ind.) – The Indiana Family and Social Services Administration has submitted its application for a 10-year extension of the Healthy Indiana Plan, the state’s Medicaid alternative program for low-income, non-disabled adults. This week, the U.S. Centers for Medicare and Medicaid Services notified FSSA that it has completed its preliminary review of the application, which prompts the start of a 30-day federal public comment period.
The Healthy Indiana Plan was first launched to a limited number of Hoosiers in 2008 and expanded to cover any eligible adult in 2015 as an alternative to traditional Medicaid expansion.
Today, HIP provides crucial health insurance coverage and access to quality care and services to more than 400,000 Hoosiers. Typically, the state’s waiver to renew HIP is reviewed and approved every three to four years. For the first time, Indiana is pursuing a historic 10-year waiver, allowing key staff to spend more time operating and continually improving HIP so that it meets its goals, such as helping members manage their own health coverage and make choices as consumers of health care.
With this waiver application, Indiana solidifies its commitment to HIP as the model for health coverage reform in Indiana for the foreseeable future. Therefore, FSSA does not have plans to seek a Medicaid block grant at this time. Last month, CMS announced new options for states to seek waivers to innovative adult health coverage programs similar to the way Indiana has done with HIP.
“We are focused on the renewal of our existing waiver, which already contains many of the elements CMS recently encouraged states to pursue,” said Jennifer Sullivan, M.D., M.P.H., FSSA secretary. “While we’re excited that the recently announced program may help other states discover new avenues for health reform within their Medicaid programs, we feel the model we already have is the right one for Indiana.”
The extension request asks CMS to approve HIP through December 2030, locking in the plan that the state has achieved through a decade of data analysis, member and stakeholder feedback, and external reviews. In the current request, Indiana is asking for more flexibility in the contributions and copayments assessed, subject to capped amounts. The state is also asking to extend newer components of HIP, such as treatment for substance use disorder and serious mental illness, for five years.
FSSA also has an application pending with CMS to establish a new program to complement HIP, the HIP Workforce Bridge. HIP Workforce Bridge is designed to financially support HIP members who are transitioning to employer insurance or other health coverage.
Anyone wishing to provide comments on the HIP waiver application can do so at this link on Medicaid.gov where it is posted for a 30-day federal public comment period.

 Gov. Braun Recognizes Over 25,000 EMS Professionals for EMS Week 2026
Gov. Braun Recognizes Over 25,000 EMS Professionals for EMS Week 2026
 Riverboat Rides Raise Funds for INcompass Health Switzerland Co. Food Bank
Riverboat Rides Raise Funds for INcompass Health Switzerland Co. Food Bank
 From Bright to Bestseller Dreams: Local Author Writes Thriller Series Around Moores Hill
From Bright to Bestseller Dreams: Local Author Writes Thriller Series Around Moores Hill
 INDOT: State Road 46 Bridge Project Will Run Into Fall
INDOT: State Road 46 Bridge Project Will Run Into Fall
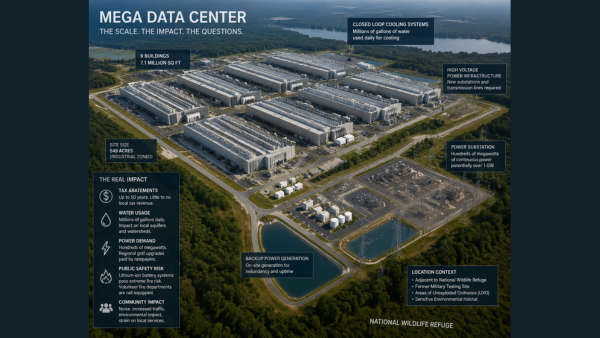 Jefferson County Data Center Sparks Community Debate
Jefferson County Data Center Sparks Community Debate
 Jared Leiker Named District 10 High School Principal of the Year
Jared Leiker Named District 10 High School Principal of the Year














Comments
Add a comment